
Palliative care is a relatively new medical specialty rapidly expanding over the past decade. Since the year 2000, the number of hospitals with inpatient palliative care teams has increased by nearly 148%, including 66% of all hospitals over 50 beds 1. Despite this rapid growth, there are not enough specialists in palliative care to meet the growing need and all providers could benefit from generalist training in palliative care principles (Quill, & Abernathy, 2013). Palliative comes from the Latin root “Palliere” which means “to cloak.” The practice of palliative care represents the interdisciplinary care that aims to relieve suffering, improve quality of life, optimize function, and promote both autonomous and shared decision-making for patients (and their families) with serious illness. Care is holistic, addressing not only the medical illness but also the psychological, social, and spiritual dimensions of serious illness. For a person to feel well, all aspects of suffering must be addressed. While a cure may not always be tenable at the end stage of chronic disease or a terminal illness, the management of troublesome symptoms may relieve suffering and improve a patient’s quality of life. This article serves to define palliative care, summarize the differences and similarities of palliative care and hospice, generalist vs. specialist care, prognostication, symptom management, advance care planning and the overall benefits of palliative care.
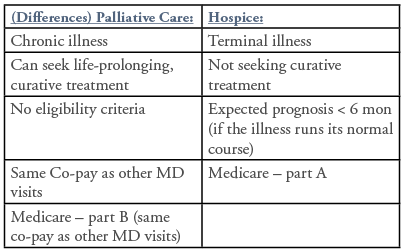
Palliative Care vs. Hospice:
The distinguishing and often misunderstood feature of palliative care is that it can occur in conjunction with life prolonging and curative therapy. In other words, all hospice care is palliative, but not all palliative care is hospice. For example, patients with cancer may receive surgery, chemotherapy, and radiation with the intent to cure, and still qualify for and benefit from palliative care services. A landmark trial in the New England Journal of Medicine demonstrated “among patients with metastatic non–small-cell lung cancer, early palliative care led to significant improvements in both quality of life and mood. As compared with patients receiving standard care, patients receiving early palliative care had less aggressive care at the end of life but longer survival.” 2 Hospice falls under the umbrella of palliative care, and referral is appropriate when patients have a terminal diagnosis and death is expected within 6 months. Patients and health care providers often need reassurance that a referral to hospice is not “giving up hope”. Studies show patients receiving hospice care, when compared to hospitals, nursing homes, and traditional home care, have significantly improved symptoms (less pain, shortness of breath, fatigue), better quality of life, better caregiver spiritual and emotional support, and decreased complex grief among decedents associated with intensive care unit deaths. 3, 4 Hospice care actually results in a mean overall survival benefit of 29 days for many cancers and congestive heart failure (CHF), with a benefit of the reduced cost of hospital care. 5
(Similarities) Palliative Care and Hospice: interdisciplinary, holistic, patient and family focused, quality of life, communication, symptom management
Locations of Care:
The ultimate goal is to offer palliative care in any location in which a patient would need services.
Meet the Team:
Palliative care is delivered utilizing an interdisciplinary model. A team may include physicians, advanced provider practitioners, and nurses in various medical specialties, as well as social workers, chaplains, mental health providers, and community members. While some members of the team may be palliative care specialists, others represent a group of multifaceted expertise who contribute to the overarching goals of optimizing palliation (Quill & Abernathy, 2013). Listed below are the distinctions between generalist and specialist palliative care. 6
Consult Etiquette:
When a consultation is requested, providers exchange information about what is most important to accomplish during the visit from the standpoint of the referring clinician. This discussion with the referring clinician should include whether the patient and/or family are aware of the palliative consult, the content of previously discussed management and planning and whether matters of a sensitive nature are acceptable to discuss with the patient at the initial visit. Following a detailed assessment which includes a thorough chart review of the patient’s history, symptoms, and examination; the provider should prepare to engage the patient and their family. An appropriate location should be identified to discuss desired goals for management. A private setting with minimal distraction is ideal and an invitation should be made in advance to ensure all surrogate decision members are present. Consults are typically standardized within institutions and include: symptom management, prognosis, goals of care, advance care planning such as code status/completion of advance directives, psychosocial and spiritual support. Knowledge of aggressive pain and non-pain symptom management and its relationship to the social and practical needs of caregivers, and the relationship of spiritual and existential suffering is a necessary component of palliative care. 7 Engaging other members of the patient’s care team to gather additional treatment specific considerations and prognosis may be indicated. In complex cases, additional consultation by a specialist may prove necessary to facilitate care (e.g. heart transplant and/or heart pump assist devices from a cardiologist). Specialist-level skills include advance care planning, status of life sustaining therapies (ie code status), roles and responsibilities of surrogate decision-makers, ethical considerations, provider-patient shared decision making, legal requirements for use of controlled substances, pronouncing death, and request for autopsy and organ donation . 7
Symptom Management:
Patients with serious illness or in advanced stages if their co-morbidities eventually develop symptoms related to their disease. These symptoms can decrease quality of life for the patient and caregivers by impeding sleep, work, eating, self-care, mentation and participation in enjoyable activities. Patients and caregivers may have a poor understanding of the disease, unrealistic expectations of care, and low health literacy. Health care treatment can be fragmented with poor communication or resources to prepare patients and families for the end of life. This paradigm frequently ends in a systematic default to emergent and aggressive care in response to an overestimated legal risk, fear, or discomfort with death. 8 The result is non-beneficial care in elderly or terminal patients with serious illness including escalation of care at the end of life, including repeated and potentially preventable emergency room visits, hospital readmissions, burdensome treatments and interventions and death in the hospital intensive care unit. In some situations, these interventions only serve to prolong the dying process. This invasive trajectory can create unnecessary suffering of patients, caregivers, health care providers, and can threaten the stability of the healthcare system at large. When provided with prognosis and assessments of the risks and benefits of treatment, many patients chose to focus on care that preserves the quality of their life, even if the quantity of life may be limited. Studies show the majority of patients, families, and even health care providers want symptoms managed, to be informed of their prognosis, treated as a whole person, and to avoid artificial life support as death approaches. 9 Palliative symptoms include pain and non-painful symptoms such as shortness of breath, nausea, vomiting, constipation, anorexia, fatigue, insomnia, anxiety, depression, and delirium. Pain, and most other symptoms, are subjective. That is, individuals can experience the same painful stimulus or injury differently because of genetic variance underlying physiologic differences in pain perception and emotional, cultural or spiritual influence. Pharmacologic treatments can also include complementary and alternative medications, such as vitamins and herbs. Non-pharmacologic care includes arranging sessions with a mental health professional, physical/occupational/speech therapy, spiritual/cultural advisor, meditation (or other forms of therapy that triggers the relaxation response such as repetitive prayer, guided imagery, Tai Chi, Yoga), arts in medicine, animals in medicine, diet, and exercise.
Prognostication:
Good communication and shared informed decision making is a cornerstone of palliative care. Ensuring that patients and families understand their diagnosis and prognosis is imperative, as this allows individuals to make informed decisions about the benefits and burdens of medical interventions. Prognosis is based not only on the disease, but on age, functional status, comorbidities, and psychosocial support. Physicians overestimate prognosis and the longer they have cared for a patient, the greater the overestimation (Christakis & Lamont, 2000). If care will not add to the quantity or quality of life, its benefit should be questioned. Based on cultural background and experience individuals develop a set of values that influences their choices in medical care. These values vary individually and are as unique as each patient. Values and priorities may change as the disease progresses. Palliative care specialists set aside personal values and listen openly to determine the patient-centered values and goals of care. A key role of palliative care is to help facilitate honoring a patient’s treatment preferences. At times the palliative care team is called to assist in resolving conflicts in goals of care between patients and family, between patients and health care providers. Ethics consultation may be helpful when conflict arises and teams need to ensure all avenues legally, medically, ethically have been explored to honor a patient’s autonomy. An example is a family is unable to make a decision for their loved one regarding life-prolonging versus comfort care. Physicians often assume patient’s goal of care is life prolongation and the medical system defaults to aggressive care for all individuals, even if this would not result in an acceptable quality of life for an individual base their values. This comes from an underlying culture of medical training that illness and death represent a “failure”.
What is your patient’s goal of care?
Advance Care Planning:
Advance care planning is the foundation of palliative care and a basic skill required by all healthcare providers. The goal is to move advance care planning upstream, to outpatient clinics. Advance care planning should be initiated earlier in the trajectory of chronic illness, when patients can express their wishes and communicate them to their loved ones. All providers need to create processes within their practice for engaging in these important conversations and understanding patients’ wishes. Contrary to expectations, patients appreciate talking to their healthcare provider about advance care planning. Having the conversation in a non-emergency setting is much preferred to waiting until the patient’s arrival at hospital emergency departments when the patient can no longer voice their wishes. The goal is to normalize advance care planning conversations and assist patients to carefully consider and document healthcare preferences prior to crisis situations. Completion of advance directives enables individuals to maintain their wishes for care, even during a period of incapacity, which can occur after unexpected illness, accident, or during the end of life. Completion of documents is typically not an isolated event, but a process over time to be revisited periodically and updated based on disease progression. Once advance directives are complete, there may be barriers in implementing them in critical situations, including availability to treating physicians and institutions, vague and legalistic language, proxy availability and use of substituted judgment and honoring previously expressed wishes to make decisions according to what the patient would have wanted. As you can imagine, system wide approaches in addition to palliative care consultation are needed to successfully implement routine completion, collection, and storage of advance directives. The Physician’s Order for Life Sustaining Treatment (POLST) is legally valid document in several other states to direct current treatments, created with the intention of addressing the issue of portability between inpatient and outpatient settings and between institutions specifically for patients with serious illnesses. It is legally valid in and out of the hospital and specific to the patient’s treatment preferences. For more information and to be part of initiatives to implement the POLST in Florida, please visit its website listed below.
Quality Improvement:
Research, education, and policy making are included in the mission of academic palliative care. Recently published by the Institute of Medicine, and receiving national attention, is a report entitled Dying in America. The report outlines the importance of improving quality and honoring individual preferences near the end of life. “Health system managers, payers, and policy makers have a responsibility to ensure that end of life care is compassionate, affordable, sustainable, and of the best quality possible”. A substantial body of evidence demonstrates that this type of care is within reach and provided by palliative care. In summary, palliative care is “associated with higher quality of life, including better understanding and communication, access to home care, emotional and spiritual support, well-being and dignity, care at the time of death, and lighter symptom burden. Some evidence suggests that, on average, palliative care and hospice patients may live longer than similar ill patients who do not receive such care” all for a cost savings to the system. 10
Summary of Benefits:
References:
1 The Advisory Board Company PEC. Realizing the Full Benefit of Palliative Care Briefing Palliative Care Executive Committee. 2013:9.
2. Temel, Jennifer MD, Greer, Joseph, Ph.D., et al. Early Palliative Care for Patients with Metastatic Non–Small-Cell Lung Cancer. N Engl J Med 2010; 363:733-742
3. Morrison RS, MD. Director, National Palliative Care Research Center; Outcomes and Quality Standards. Center for Advanced Palliative Care; 2014; Orlando 2014. Luckett. BMC Health Services Research; 2014. Gelfman LP MD, Morrison RS. JPSM. 2008.
4. Kross EK, Engelberg RA, Gries CJ, Nielsen EL, Zatzick D, Curtis JR. ICu care associated with symptoms of depression and posttraumatic stress disorder among family members of patients who die in the icu. Chest. 2011;139(4):795-801.
5. Kelly AS DP, Morrison RS. Health Affairs; 2013.
6. Generalist Plus Specialist Palliative Care (N Engl J Med 2013;368:1173-75)
7. Home / Journals / AFP / Vol. 73/No. 6(March 15, 2006) / Practice Guidelines: Guidelines for Delivering Quality Palliative Care
8. Cooper, Zara, MD, Courtwright, Andrew, MD et al. Pitfalls in Communication That Lead to Nonbeneficial Emergency Surgery in Elderly Patients with Serious Illness, Annals of Surgery, Volume 260, number 6, December 2014.
9. Factors considered important at the EOL by pts, families, physicians, and other care providers. JAMA 2000
10. POLST Web Site: http://www.polst.org/about-the-national-polst-paradigm/