- Archives
- 2010 Volume 7 Number 4 October- December
- The Radiation Overdose Sentinel Event
The Radiation Overdose Sentinel Event
Libby Brateman, PhD,
FACR, FAAPM
Associate Professor, College of Medicine, Department of Radiology and
Affiliate Associate Professor, College of Engineering, Department of Nuclear and
Radiological Engineering

The Joint Commission has defined a radiation overdose sentinel event to be a patient peak skin dose of 15 Gy from fluoroscopic procedures within a 6-to-12 month period. The Joint Commission FAQ sheet on the radiation overdose sentinel event includes neonatal serum bilirubin > 30 mg/dl and prolonged fluoroscopy with cumulative dose > 1500 rads [15 Gy] to a single field or any delivery of radiotherapy to the wrong region or > 25% above the planned dose. The commonality among these three situations is:
These events could be associated with death or major permanent loss of function,
These outcomes often do not occur for months or years after the event itself, and
These events are considered to be preventable.
Therefore, after identification of any of these events, hospitals are required to conduct a root cause analysis and are encouraged to report the event even though the outcome has not yet become evident. The FAQ sheet goes on to say “the purpose of the Sentinel Event Policy is to promote improvement in patient safety, not to regulate practice. The parameters defining these sentinel events were intentionally selected to identify only the most extreme cases—those that should never occur.”
One might wonder why fluoroscopic radiation at this skin dose level was chosen to be defined as a sentinel event, particularly because of The Joint Commission’s definition of a sentinel event:
“A sentinel event is an unexpected occurrence involving death or serious physical or psychological injury, or the risk thereof. Serious injury specifically includes loss of limb or function. The phrase, “or the risk thereof” includes any process variation for which a recurrence would carry a significant chance of a serious adverse outcome. Such events are called “sentinel” because they signal the need for immediate investigation and response.”
It may come as a surprise that fluoroscopic procedures have the potential to cause risk of serious injury. Certainly the media have been announcing the extreme situations in which radiation from diagnostic CT scans has caused patient injuries. (See, for example “Radiation Overdoses Point up Dangers of CT Scans,” Oct. 15, 2009, and “After Stroke Scans, Patients Face Serious Health Risks,” July 31, 2010, in The New York Times.) In these situations, patients have suffered hair loss and attained the potential for cataracts. Perhaps hair loss is not seen as a serious injury in a medical sense, but when the patient is an elementary school teacher with a student who vomits because of seeing her patchy hair loss, the impact is not inconsequential.
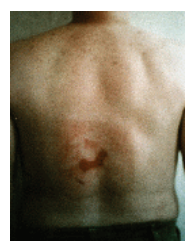
The fact is that any user of fluoroscopes has the potential to cause, not only hair loss, but also cutaneous radiation injury (CRI) that includes serious skin burns that often do not show up until sometime after the patient has been discharged. Injury to the skin may occur and appear to heal but then return with a vengeance some time later. See, for example, the classic images on the FDA website (http://www.fda.gov/Radiation EmittingProducts/ RadiationEmittingProductsandProcedures/ MedicalImaging/MedicalX-Rays/ucm116682.htm) that were presented in a 1995 medical conference.
——–
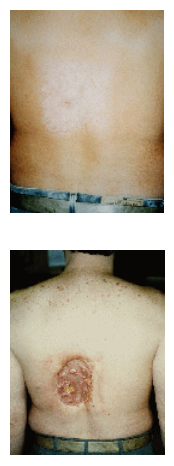
The top photo ti the left is at 6-8 weeks following multiple procedures involving angiography and angioplasty. The shape of the radiation field on the skin of the patient is apparent. The center photo at 16-21 weeks shows only a small ulcerated area present, with the appearance of general healing. However, the bottom photo, taken at 18-21 months post-procedures, shows tissue necrosis that required skin grafting. Specific dose information was not available, but the estimated dose was greater than 20 Gy.
All radiation injuries, indeed all serious injuries and illnesses associated with the use of medical devices, are supposed to be reported under the Safe Medical Devices Act of 1990. The Joint Commission encourages voluntary reporting of sentinel events.
FDA concerns led to a Public Health Advisory (9/30/1994) that identified procedures that typically involve extended fluoroscopic times:
● percutaneous transluminal angioplasty (coronary and other vessels)
● radiofrequency cardiac catheter ablation
● vascular embolization
● stent and filter placement
● thrombolytic and fibrinolytic procedures
● percutaneous transhepatic cholangiography
● endoscopic retrograde cholangiopancreatography
● transjugular intrahepatic portosystemic shunt
● percutaneous nephrostomy
● biliary drainage/urinary/biliary stone removal (http://www.fda.gov/MedicalDevices/ Safety/AlertsandNotices/ PublicHealthNotifications/ucm063084.htm)
The FDA stated in the above advisory: “Physicians performing these procedures should be aware of the potential for serious, radiation-induced skin injury caused by long periods of fluoroscopy during these procedures. It is important to note that the onset of these injuries is usually delayed, so that the physician cannot discern the damage by observing the patient immediately after the treatment.”
Fluoroscopy time is not the only parameter that affects skin dose. Studies with high doses could almost always have been performed with lower doses by the operator knowing how the equipment was designed to work and using features associated with lower radiation doses by optimizing work practices. Physicians who use fluoroscopy equipment throughout the hospital need to have as much knowledge as possible about how to use the equipment. Starting with the most basic imaging principles, such as which end of the C-arm fluoroscope is the x-ray tube, and which end should be kept as close to the patient as possible (the imager), all physicians who operate fluoroscopes need to know how to keep the radiation doses to their patients, other staff and themselves as low as reasonably achievable in the process of making images with appropriate image quality.
How do we know the radiation dose? All fluoroscopes manufactured after June 10, 2006 are required by the FDA to have dose meters installed on them. Some earlier (“vintage”) equipment may also have these meters, and some can be upgraded to have meters installed. With such meters, the dose can be monitored during the study, and then a value can be obtained after the study. This meter value is not actually the patient skin dose, but instead, this reported value can be used by a medical physicist in conjunction with various additional parameters when a personalized estimate of the patient peak skin dose is necessary. However, dose meter values can be used as first estimates, and they can be tracked for patients so that alerts can identify patients whose peak skin doses are likely to be high.
What is the significance of the 15-Gy dose level at which The Joint Commission set the threshold for the radiation sentinel event? The CDC has a “Radiation Fact Sheet for Physicians” that gives detailed information regarding CRI and what effects to expect at various radiation levels. These effects are divided into grades of injury, and the CDC separates a Grade I CRI from a Grade II injury at 15 Gy. (http://emergency.cdc.gov/ radiation/criphysicianfactsheet.asp) According to this report, radiation effects include: edema of subcutaneous tissues and blisters with moist desquamation at 5-6 weeks post-exposure, blood vessel damage at 10-16 weeks post-exposure, with possible ulceration; and late effects of recurrence of ulceration and possible tissue necrosis as well as telangiectasia up to 10 years later.
The Joint Commission radiation sentinel event definition, therefore, is at the break-point between the CDC-defined Grade I and Grade II CRI. This definition refers to a peak skin dose in a single field over a period of 6 months to a year, because “skin sensitivity is, to a degree, repairable.” Radiation oncologists are well aware that radiation effects can be controlled by a well-planned fractionation regimen, but unexpectedly lengthy fluoroscopic procedures do not fall in that category. Note that the sentinel event is defined for the peak skin dose received from fluoroscopic procedures, but the patient’s skin effects are related to the total dose received by that same portion of skin from all x-ray procedures, including CT and radiography in general—and including the doses from x-ray studies done elsewhere. Note also that, while the skin is the organ of interest for the sentinel event definition, doses to other sensitive organs might be of concern as well. In fact, some organs, such as the lens of the eye, can be damaged at doses much lower than 15 Gy, depending on the fractionation.
The Department of Radiology at Shands UF has been developing procedures for monitoring and tracking patient radiation doses and a policy for managing high doses with the goal of preventing CRI. A review has found that high peak skin doses involving embolization procedures place patients who require multiple embolization procedures at a higher risk.
The Joint Commission understands that “The terms ‘sentinel event’ and ‘medical error’ are not synonymous; not all sentinel events occur because of an error and not all errors result in sentinel events.” Depending on a patient’s diagnosis, high peak skin doses may be a necessary and unavoidable part of their treatment regimen, and patients should be informed of the potential for adverse radiation effects when they are known to exist.
References: (http://www.jointcommission.org/NR/ rdonlyres/10A599B4-832D-40C1-8A5B-
5929E9E0B09D/0/Radiation_Overdose.pdf) (http://www.jointcommission.org/NR/ rdonlyres/F84F9DC6-A5DA-490F-A91F-
A9FCE26347C4/0/SE_chapter_july07.pdf


 ——–
——–